Skincol® is a tried and tested assistant in the treatment of both chronic and acute wounds, radically accelerating their healing.
The results of clinical tests and studies have confirmed that Skincol® is a highly effective cream patch suitable for a wide range of skin wounds from grazes, slicing injuries and surgical wounds to burns and poorly healing varicose ulcers and bedsores.
Sucralfate has more than 100 studies
Some important clinical studies:
Hippokratia. 2013 Apr;17(2):126-9.
Sucralfate gel as a radioprotector against radiation induced dermatitis in a hypo-fractionated schedule: a non-randomized study.
Kouloulias V1, Asimakopoulos C1, Tolia M1, Filippou G1, Platoni K1, Dilvoi M1, Beli I1, Georgakopoulos JPatatoukas GKelekis N
Author information
Abstract
External beam radiotherapy with high doses provokes many acute skin reactions, such as erythema and moist desquamation. Many topical preparations are used in radiation oncology departments in the skin care. Sucralfate humid gel, a colloidal physical form of the anti-ulcer drug sucralfate, promotes epithelial regeneration and activates cell proliferation. Based on this knowledge, we performed a non-randomized clinical trial to evaluate the efficacy of topical sucralfate gel in 30 breast cancer patients receiving postoperative accelerated hypofractionated photon beam therapy. The comparison was performed with 30 patients as historical controls. The acute reaction of the skin was significantly lower in the group receiving the sucralfate gel (p<0.05, Mann Whitney test), while 90% of the patients had no evidence of radiation induced skin toxicity. There was no sucralfate gel related toxicity reported by any patient in this study. More patients in a randomized way are needed for more definite results.
KEYWORDS:
Oral; cancer; chemotherapy; mucositis; radiotherapy
Topical treatment of chronic venous ulcers with sucralfate: a placebo controlled randomized study.
Randomized controlled trial
Tumino G, et al. Int J Mol Med. 2008.
Show full citation
Abstract
Venous leg ulcers are an important medical issue due to their high incidence in the elderly and the lack of a standard curative approach. Apart from surgical therapy, different medical treatments to effect ulcer wound repair and regeneration are currently being investigated. Sucralfate is a cytoprotective agent employed to prevent or treat several gastrointestinal diseases such as gastroesophageal reflux, gastritis, peptic ulcer, stress ulcer and dyspepsia. In this study we evaluated the efficacy, safety and tolerability of topical sucralfate (SUC-LIS 95) on the healing of chronic venous leg ulcers in 50 patients by a double-blind, placebo-controlled, randomized study. Our results indicated that the daily application of SUC-LIS 95 to non-infected post-phlebitis/vascular ulcers, for a median period of 42.0 days, led to complete healing in 95.6% of patients, against only 10.9% of cases with a matched placebo. A significant improvement was obtained in the SUC-LIS 95-treated patient group with regard to local tissue inflammation as well as pain and burning, and consequently, in ulcer size and the evolution of granulation tissue. Our findings were corroborated for selected patients by the morphological analysis of biopsies obtained before and after treatment. Using ultrastructural analysis we demonstrated that the topical use of SUC-LIS 95 was able to affect neoangiogenesis, increase wound contraction, promote re-epithelialization of the wound area and diminish the inflammatory reaction. Overall, our results indicated that patients with chronic venous ulcers show improvement after the use of topical sucralfate.
PMID 18575771 [PubMed - indexed for MEDLINE]
Dis Colon Rectum. 2011 Jun;54(6):699-704. doi: 10.1007/DCR.0b013e31820fcd89.
Topical sucralfate treatment of anal fistulotomy wounds: a randomized placebo-controlled trial.
Gupta PJ1, Heda PS, Shrirao SA, Kalaskar SS.
Author information
Abstract
BACKGROUND:
Sucralfate is a cytoprotective agent which adheres to mucoproteins and forms a protective barrier at wound sites. In oral form it is a common ulcer medication, and as a topical preparation it has been used to treat a wide variety of wounds.
OBJECTIVE:
The present study was designed to evaluate the effectiveness and safety of topical sucralfate in wound healing after anal fistulotomy.
DESIGN:
Double-blind, randomized controlled study comparing topical application of sucralfate or placebo.
SETTING:
Private outpatient clinic specializing in anorectal disease in Nagpur, India.
PATIENTS:
Patients with a wound length of at least 5 cm after low anal fistulotomy were eligible for the study.
INTERVENTION:
Patients were randomly assigned to receive ointment containing 7% sucralfate or a placebo ointment consisting of petroleum jelly. Patients were instructed to apply approximately 3 g of ointment to the wound twice daily after a sitz bath for 6 weeks or until the wound had healed.
MAIN OUTCOME MEASURES:
The wounds were examined by a blinded independent observer at 2, 4, and 6 weeks after the operation. The primary end point was the proportion of patients with wounds that had completely healed. Secondary end points included amount of mucosal covering (scored by the observer), adverse events, and postoperative pain (self-rated on a visual analog scale).
RESULTS:
Of 80 participants (29 women, 51 men; median age, 23 (range, 17-49) years), 76 participants completed the trial (sucralfate, 39; placebo, 37). At 6-week follow-up, complete wound healing was achieved in 37 patients (95%) in the sucralfate group and 27 patients (73%) in the placebo group (P = .009). Mucosal coverage of the wound was significantly greater with sucralfate than with placebo at each measurement point (P = .01). No adverse events were observed. Postoperative pain scores were significantly lower for sucralfate than for placebo at 2 and 4 weeks after the start of treatment.
LIMITATIONS:
Wound tissue specimens were not available for morphological and ultrastructural analysis.
CONCLUSIONS:
The results of this study add support to the evidence that topical sucralfate is a safe and effective method for promoting mucosal healing and for providing analgesia during wound treatment. Patients undergoing anal fistulotomy can benefit from the use of topical application of sucralfate.
PMID: 21552054 DOI: 10.1007/DCR.0b013e31820fcd89
Recent Pat Inflamm Allergy Drug Discov. 2010 Jan;4(1):25-36.
Topical use of sucralfate in epithelial wound healing: clinical evidences and molecular mechanisms of action.
Masuelli L1, Tumino G, Turriziani M, Modesti A, Bei R.
Author information
Abstract
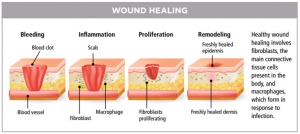
Sucralfate is a basic aluminium salt of sucrose octasulphate which was orally employed for prevention and treatment of several gastrointestinal diseases including gastroesophageal reflux, gastric and duodenal ulcer. Recent studies have employed sucralfate as a topical drug for the healing of several types of epithelial wounds such as ulcers, inflammatory dermatitis, mucositis and burn wounds. Epithelial wound healing is a well orchestrated process involving hemostasis, inflammatory reaction, cell proliferation and tissue remodelling which leads to granulation tissue development and filling of the wound space. This report will review clinical evidences on the use of topical sucralfate for the management of epithelial lesions and deal with the current knowledge on the molecular mechanisms of action of this compound towards the epithelial wound healing process and will also discuss relevant patents.
PMID: 19832693
[PubMed - indexed for MEDLINE]
Dis Colon Rectum. 2008 Feb;51(2):231-4. Epub 2007 Dec 18.
Topical sucralfate decreases pain after hemorrhoidectomy and improves healing: a randomized, blinded, controlled study.
Gupta PJ1, Heda PS, Kalaskar S, Tamaskar VP.
Author information
Abstract
PURPOSE:
Oral and topical sucralfate is regularly used in ulcers of gastrointestinal tract, vaginal and perianal excoriations, and radiation burns. This study was designed to determine whether there was any advantage of topical application of sucralfate in reducing postoperative pain and promoting wound healing after open hemorrhoidectomy in patients with Grades III or IV hemorrhoids.
METHODS:
A total of 116 patients were randomly assigned to receive sucralfate cream (sucralfate group) or placebo cream (control group) applied to the surgical site. Weekly pain score was evaluated by using Visual Analog Scale. The amount of analgesic tablets consumed in each week also was assessed. At the end of four weeks, two independent surgeons assessed the wound healing.
RESULTS:
There was no significant difference in age, gender distribution, and number of excised hemorrhoid piles between the two groups. Patients in the topical sucralfate group experienced significantly less pain at Day 7 (Visual Analog Scale +/- standard error of the mean, 3.7+/-0.3 vs. 6.1+/-0.7; P<0.002) and at Day 14 (1.6+/-0.2 vs. 3.1+/-0.6; P<0.01). Likewise patients who received sucralfate cream used less analgesic tablets compared with the placebo group. In the sucralfate group, the overall wound healing ranked significantly better than in controls (P<0.02).
CONCLUSIONS:
Topical sucralfate significantly reduces pain at Days 7 and 14 after hemorrhoidectomy and promotes faster wound healing compared with that of a placebo.
Comment in
PMID: 18095028 DOI: 10.1007/s10350-007-9092-4
J Clin Rheumatol. 2006 Dec;12(6):282-6.
Behçet disease: recommendation for clinical management of mucocutaneous lesions.
Lin P1, Liang G.
Author information
Abstract
Mucocutaneous lesions are the most common manifestation of Behçet disease. These lesions can often become refractory to multiple treatments and present challenges to physicians. In this article, different treatments for mucocutaneous lesions in Behçet disease are reviewed and discussed. Topical or intralesional corticosteroids, oral pentoxifylline, sucralfate, dapsone, colchicine, and systemic low-dose corticosteroids, used either alone or in combination, are safe and having varying evidence for effect in mild to moderate mucocutaneous disease. Azathioprine or methotrexate can be used if the lesions are refractory to the previously mentioned therapies. Tumor necrosis factor (TNF) inhibitors such as infliximab or etanercept should be considered as the next step in the treatment if azathioprine or methotrexate fails. Tacrolimus, cyclosporine, and interferon-alpha-2a should be used generally only if TNF inhibitors have failed as a result of their toxicities.
PMID: 17149058 DOI: 10.1097/01.rhu.0000249894.03016.de
Burns. 2001 Aug;27(5):465-9.
Topical use of Sucralfate Cream in second and third degree burns.
Banati A1, Chowdhury SR, Mazumder S.
Author information
Abstract
This clinical study was undertaken to test the efficacy of topical Sucralfate Cream in second and third degree burns. Topical Sucralfate Cream has been used on a wide variety of lesions from radiation proctitis and dermatitis to keratoconjunctivitis with remarkable results. The study was carried out in two phases. The first phase comprised 60 patients, 30 of whom were treated with Sucralfate Cream while the other 30 were treated with other topical antimicrobial agents. Twenty-one of the patients in the study group had second-degree burns and nine patients' third degree burns. In the second phase, a double blind study was carried out on 25 patients where one area of burns was treated with Sucralfate Cream while another control area of the same patient was treated with a placebo ointment, containing the excipients used during preparation of the Sucralfate Cream, without Sucralfate. In the first phase, it was seen that the period of epithelialisation of second degree burns in the study group treated with Sucralfate Cream was 18.8 days compared with 24.6 days with other topical agents. This difference is statistically significant with a P value of <0.00001. In the double blind study, also healing in the areas treated with Sucralfate was more rapid than those treated with bland placebo ointment. The difference in the two rates of healing was statistically significant with a P value of 0.00067. Histopathological studies were also carried out in 10 patients of phase I of the trial. Sucralfate Cream promotes rapid epithelialisation of second degree burns with minimal said effects and offers another topical agent in the burn care specialist's armamentarium.
PMID: 11451599
[PubMed - indexed for MEDLINE]
Clin Exp Dermatol. 2000 Nov;25(8):584-8.
Topical sucralfate in the management of peristomal skin disease: an open study.
Lyon CC1, Stapleton M, Smith AJ, Griffiths CE, Beck MH.
Author information
Abstract
Dermatoses affecting the skin around stoma sites are common and difficult to treat. We have investigated the effectiveness of topical sucralfate in the management of peristomal dermatoses in adults using an open study design. Apart from forming a physical barrier to further irritation, sucralfate binds to basic fibroblast growth factor preventing its degradation and thereby promotes healing. In eight out of nine patients with faecal or urine erosions, daily, topical sucralfate treatment was associated with healing within 4 weeks. There was limited or no response to treatment in a further nine patients with traumatic ulcers, excoriated dermatitis or pyoderma gangrenosum. Topical sucralfate represents a safe, inexpensive and effective therapeutic intervention, particularly for those patients with high output or short stomas where repeated stoma leakage may be unavoidable.
PMID: 11167966
[PubMed - indexed for MEDLINE]
Arch Dermatol. 1999 May;135(5):529-32.
The use of sucralfate suspension in the treatment of oral and genital ulceration of Behçet disease: a randomized, placebo-controlled, double-blind study.
Alpsoy E1, Er H, Durusoy C, Yilmaz E.
Author information
Abstract
OBJECTIVE:
To determine the efficacy of topically applied sucralfate suspension in the treatment of oral and genital ulceration of Behçet disease.
DESIGN AND SETTING:
A randomized, placebo-controlled, double-blind study at a university referral center.
PATIENTS:
Forty patients with Behcet disease were included in the study.
INTERVENTION:
Patients were given topical sucralfate or placebo 4 times a day for 3 months and examined clinically at biweekly intervals.
MAIN OUTCOMES MEASURES:
For each lesion, the mean frequency, healing time, and pain were evaluated during the pretreatment, treatment, and follow-up periods. No patients were given any concurrent disease-specific or immunosuppressive topical and systemic drugs during the 9-month study period.
RESULTS:
Of the 40 patients included in the study, the results in 30 patients (16 patients treated with sucralfate and 14 patients treated with placebo, ranging in age from 16 to 52 years [mean+/-SD age, 34.3+/-8.1 years]) were evaluable for efficacy. Treatment with sucralfate decreased significantly the mean frequency, healing time, and pain of oral ulceration and healing time and pain of genital ulceration compared with the pretreatment period. The effectiveness of sucralfate on the frequency and healing time of oral ulceration continued during the post-treatment period. In the placebo group, no significant difference was found in measured parameters of oral and genital ulceration except the pain of the oral ulceration between the pretreatment and treatment periods.
CONCLUSION:
Our results showed that topical sucralfate suspension is an easy, safe, inexpensive, and effective treatment for oral and genital ulceration in patients with Behçet disease.
PMID: 10328192
[PubMed - indexed for MEDLINE]
Australas Radiol. 1997 Aug;41(3):270-5.
Sucralfate cream in the management of moist desquamation during radiotherapy.
Delaney G1, Fisher R, Hook C, Barton M.
Author information
Abstract
Randomized trials have shown that sucralfate is effective in the management of acute radiation reactions such as oesophagitis, mucositis and proctitis. However, at the time of commencement of the present trial, it had never been used in the management of moist desquamation of the skin. The purpose of the present study was to assess the value of sucralfate cream in the management of moist desquamation during radiotherapy. Patients who developed moist desquamation during radiation were eligible. Patients were stratified by site of radiotherapy into three groups: (i) the head and neck; (ii) the breast; and (iii) other sites. Patients were randomized to receive 10% sucralfate in sorbolene cream or sorbolene alone. Patients' pain and skin healing were assessed by using linear analogue self-assessment (LASA) scales and by serial measurement of the desquamated area. Due to poor patient accrual, the trial was terminated after 2 years and 39 patients. No statistically significant difference was found between the two arms in either time from randomization to healing or improvement in pain score. Twenty patients in the sucralfate arm took a geometric mean of 14.8 days to heal whereas 19 patients receiving sorbolene alone took a geometric mean of 14.2 days. The ratio of mean times of healing, 1.043, is not statistically different from 1 (P = 0.86; 95% CI = 0.65, 1.67). A total of 75% of the patients reported pain relief on application of either cream. Mean LASA scores for pain for each day after randomization were compared by treatment arm and there was no statistically significant difference (P = 0.32). The present trial was unable to show a difference in terms of time to healing or pain relief in the treatment of moist desquamation. The small number of patients in the trial gave a wide confidence interval for treatment difference, implying that an important effect of sucralfate has not been excluded. Given the poor accrual in the present, single-institution study, future studies may need to be multi-institutional and we encourage other centres to perform randomized trials in the management of moist desquamation.
Year : 2004 | Volume : 49 | Issue : 4 | Page : 181-183
Topical Sucralfate Versus Hydrocortisone Cream In The Management Of Diaper Dermatitis : A Randomized, Doubleblind Clinical Trial
Fariba Iraji, Asadolah Kiyani, Marzieh Rezazadehstrong>
Correspondence Address:
Fariba Iraji
Source of Support: None, Conflict of Interest: None
Topical corticosteroids are currently used for treatment of diaper dermatitis. Previous studies have shown the efficacy of sucralfate in the treatment of diaper dermatitis and contact dermatitis in peri-stomal areas. To evaluate the efficacy of topical sucralfate in comparison with hydrocortisone cream in the treatment of diaper dermatitis, the present study was under taken. In a double –blind randomized clinical trial, 64 patients with diaper dermatitis were treated with sucralfate cream 4% or hydrocortisone cream randomly. The duration of the treatment wad 8 weeks and the patients were evaluated every two weeks until complete healing. The results were evaluated by chi-square test. Complete healing (more than 50% improvement) occurred in 90.6% and partial healing (20-25% improvement) in rest of the patients in each group (p>0.05). Topical sucralfate is an effective, cheap therapeutic intervention for diaper dermatitis. Which has equal efficacy with topical hydrocortisone cream.
J Pediatr Surg. 1991 Nov;26(11):1279-81.
Topical sucralfate: effective therapy for the management of resistant peristomal and perineal excoriation.
Hayashi AH1, Lau HY, Gillis DA.
Author information
Abstract
Peristomal and perineal excoriation commonly occurs despite preventive measures. Drainage from around gastrostomy tubes or ongoing perineal soilage after a pull-through procedure can lead to chemical irritation, cutaneous denudation, and chronic discomfort. A multitude of topical agents have been tried with variable results. We present our experience using topical sucralfate. Fifteen patients with stomal or perineal skin ulceration were treated with topical sucralfate only after other agents had failed. Clinical photographs were obtained first. Sucralfate, prepared as either a powder or an emollient, was liberally applied to the affected area during diaper changes or when the stomal appliance was emptied. For tube gastrostomy sites, sucralfate was applied every 4 to 6 hours as required to maintain a visible layer. In 13 patients, complete healing occurred. Recovery time was dependent on the severity and extent of skin denudation. Partial healing occurred in one patient. In another patient, the skin excoriation healed but a residual candidal rash required addition of an antifungal agent. General observations included: (1) a lag time of 2 to 3 days before visible healing was evident; (2) healing occurred from the perimeter; (3) sucralfate was soothing and reduced discomfort; (4) it was ineffective for fungal dermatitis; and (5) sucralfate did not appear to have toxic or systemic effects. Topically applied sucralfate is soothing, safe, and effective.
PMID: 1812256
[PubMed - indexed for MEDLINE]